Septic Shock Study Guide
When EMS providers are called to treat someone experiencing signs and symptoms of sepsis, the disease process is already well on its way to creating a very sick patient. More and more studies are showing that sepsis requires rapid identification and intervention to ensure positive outcomes with our patients. Knowing this, we should be asking ourselves, what can I do to better my abilities to recognize sepsis and how can I treat it quickly?
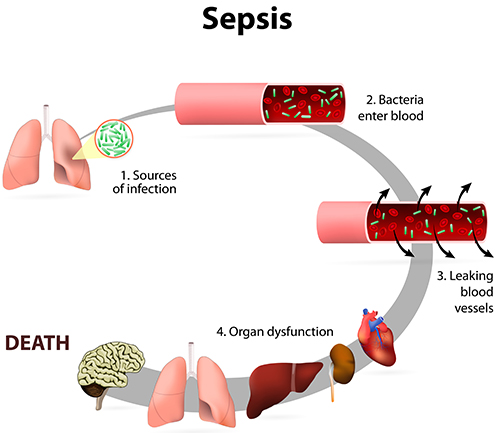
Septic shock is a type of shock that begins with an infection in the bloodstream. This infection eventually overloads the compensatory mechanisms in the body and when left untreated, leads to shock, and eventually MODS, or multiple organ dysfunction syndrome. Much like the ways in which ischemia can cause a cascade of issues in the cardiac patient, the signs and symptoms of septic shock are progressive.
How Does A Patient’s Blood Pressure Drop Because of a Bad Infection?
- In the early stages of the infection, the patient may look and act normally. They may not even be aware something is wrong. By the late stages, these patients can drop their blood pressures dramatically. The toxins that have been released into the system increase the permeability of the blood vessels. When this happens the patient’s fluid levels drop out of the vasculature in rapid succession. This loss of fluid causes their pressure to subsequently drop.
These patients will present with a wide array of symptoms based on the stage of septicemia they’re experiencing. To give an example, their skin could be flushed and hot in the early stages as their body tries to kill off the infection, then become cold and cyanotic towards the later stages. The organ system that is the most susceptible to these types of infections is the pulmonary system. It is very common for these patients to present with shortness of breath, abnormal lung sounds, and/or mild to moderate hypoxia.
When sepsis is suspected, you should let the nurses at the receiving facility know as soon as possible. We as EMS providers have the opportunity to set the tone on our arrival at the ED. Cueing the receiving facility into our suspicions can be the trigger they use to order certain tests to either confirm or deny what everyone is suspecting.
Treatment in the field will depend on your local protocols. Nationally, high-flow oxygen, large-bore IVs, and dopamine to maintain healthy blood pressure can help. Some departments are taking things one step further, they’re creating “sepsis alert” protocols to notify the receiving facilities of their patient’s potential septic conditions. To do this, crews are using sepsis meters that measure the lactic acid in the patient’s bloodstream. When your body is fighting a nasty infection, the immune system kicks into action. With sepsis, the immune system overreacts and ends up fighting itself. This releases a lot of lactate. Serial measurements of the lactate levels can help providers notify hospitals of their patient’s status, and ultimately get them definitive treatment quicker.
- Dozens of courses and topics
- State-specific requirements
- We report to CAPCE in real time