Rapid Sequence Intubation
THE INFORMATION CONTAINED IN THIS DOCUMENT SHOULD BE USED FOR TRAINING ONLY. YOU MUST FOLLOW ALL OF YOUR LOCAL PROTOCOLS WHEN PERFORMING PATIENT CARE.
In the prehospital setting, airway is your first priority when treating a conscious or semi-conscious patient (If they’re unconscious, we check circulation first to determine the need for compressions, then we check airway). Endotracheal intubation is the most definitive treatment in securing a patent airway. If a patient is having trouble keeping a patent airway, has impending respiratory arrest, or you, as a prehospital care provider, see that a patient is deteriorating and you need to definitively control their airway for them, RSI is the answer. The toughest part of RSI, is making the decision to perform the skill. The paramedic with the most experience with intubation should be the one to intubate in a situation that requires RSI. The steps for RSI are as follows:
- Set up your equipment and check to make sure it works properly
- Pre-oxygenate the patient with an airway adjunct and BVM (Bag-Valve-Mask)
- Administer your department or agency’s induction agent per local protocols
- Administer paralytic medications (again, per local protocols)
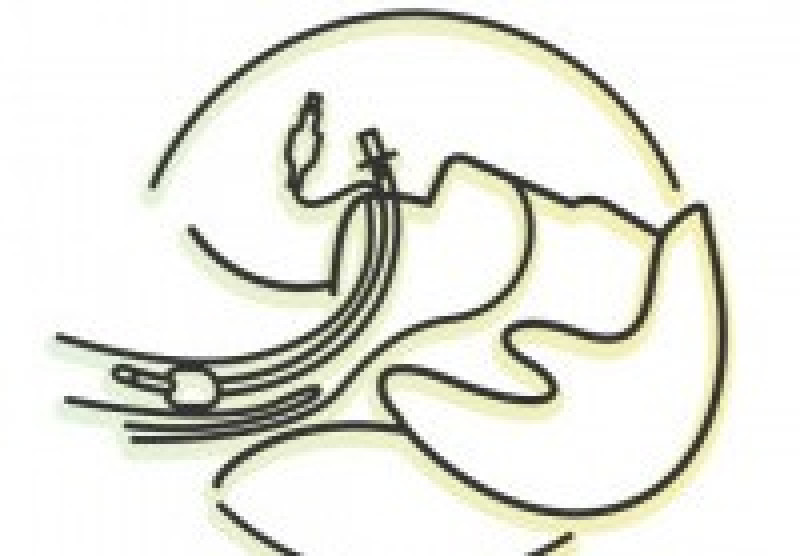
- Intubate the patient
- Confirm tube placement
- Secure the tube
- Monitor, record, and recheck vital signs every five minutes
- Monitor the patient for signs that sedative/paralytic is no longer effective
The first step in RSI is checking all of your equipment. Now is a good time to put a non-rebreather facemask on the patient to flush out nitrogen and get O2 saturation to 100%. If needed, have your partner ventilate the patient with high flow O2 at 15 liters per minute via BVM. If BVM is required, be cautious not to over-ventilate causing gastric distension, for this could cause the patient to vomit and make the intubation difficult. Cricoid pressure is a useful tool to help prevent this. Make sure to select the tube size that will allow maximum ventilation based on the patient’s anatomy. Ensure all the cuffs on the tube will inflate and stay inflated with no leaks. Next, make sure the laryngoscope is in full working order. Look for a light that is “white, tight, and bright”, with all pieces attach properly. Next, have a back-up airway device, such as a King Airway or emergency cricothyrotomy kit, at hand in case intubation is unsuccessful.
Once you have prepared all of your equipment, it is time to sedate the patient. There are several different types of induction agents used during RSI. The most common one used initially is Etomidate, but there are other drugs that can be used (Midazolam, Diazepam, Ketamine, etc.) Induction agents are solely used for their anesthetic effect, for this does not cause paralysis. It is important to know the time of onset of the induction agent before administering the paralytic.
(SIDE NOTE: If the sedative drug has not taken effect before a paralytic is administered, it is possibly that the patient is still conscious and is able to see, feel, and hear every procedure being performed, yet they’re unable to respond. Patients that have experienced this horrifying mistake state that it feels as if they were buried alive).
Now that your induction agent has taken effect, a paralytic must be administered. Some paralytic agents used in the EMS field are; succinylcholine, vecuronium, pancuronium, and rocuronium. Succinylcholine is the most commonly used paralytic agent in EMS today. This is a depolarizing neuromuscular blocking agent that prevents muscles from contracting by prolonging time during which the receptors at the neuromuscular junction cannot respond to acetylcholine. As a paramedic, it is important to know all of the drugs and how they affect the patient. When the succinylcholine takes effect, the patient can fasciculate from head to toe. Fasciculations resemble an involuntary “twitch”. The most definitive sign that the paralytic has taken effect is the relaxation of the jaw as well as the absence of respirations. Be advised, once a paralytic is administered, as a paramedic, you assume complete responsibility for maintaining a patent airway and ensuring adequate ventilations are delivered to your patient. Now that the paralytic has taken effect, it is time to intubate the patient.
During intubation, if visualizing the vocal cords is difficult, there are some skills that can help. BURP is a pneumonic that stands for; “Back, Up, Right, Pressure”. With the 2010 changes by the AHA, this skill was no longer recommended as a routine use of helping ALS providers visualize the vocal cords. That being said, there are still agencies that use this technique, so it may still be a valuable tool. This procedure is performed exactly how it sounds; have your partner apply back, up, right, pressure to the cricoid membrane which will help to visualize the vocal cords. Other tools, such as a bougie or video laryngoscope device, can be used if your agency carries them. Putting a nasal cannula on at 10-15 liters per minute may help keep the patient’s O2 saturation at adequate levels during intubation attempts. Once you have intubated your patient, confirmation that your tube placement is correct should follow immediately. Waveform capnography is the most definitive form of tube placement confirmation. Every patient’s ETCO2, as well as pulse oximetry, should be monitored to ensure adequate ventilation is being performed. An adequate ETCO2 should range from 35-45 mmHg (this can vary based on the patient’s underlying disease etiology). Also, auscultate lung sounds to make sure you have not intubated the right mainstem bronchus or the esophagus. If the intubation was successful, secure using roller gauze or a commercial tube holder. Monitor, record, and recheck vital signs every five minutes.
Once a patent airway is secured, it is crucial to keep the patient sedated and paralyzed. Signs that the sedative is no longer effective are subtle. The patient’s heart rate and blood pressure may rise, or you may notice the patient’s eyes starting to tear up. “Bucking” the tube may occur if the paralytic has worn off. This resembles gagging or coughing. Also, be sure to insert a bite block to prevent the patient from biting down on the ET tube inhibiting ventilation. Some commercial tube holders will have a bite block on them, and if not, inserting an OPA works well. Once everything is secured, maintain adequate ventilations via BVM or a ventilator, if carried by your agency. As always, make sure you follow your local protocols. The information contained in this study guide is not intended to be a substitute for your agency or department protocols. As with any ALS or BLS skill for that matter, ensure you train hard and train often. Throw curveballs in your training to prevent complacency. Remember, NEVER STOP LEARNING.
- Dozens of courses and topics
- State-specific requirements
- We report to CAPCE in real time