In this article, we are going to cover:
- The anatomy of the pelvis
- Types of pelvic fractures
- Pelvic fracture concerns
- How to manage pelvic fractures
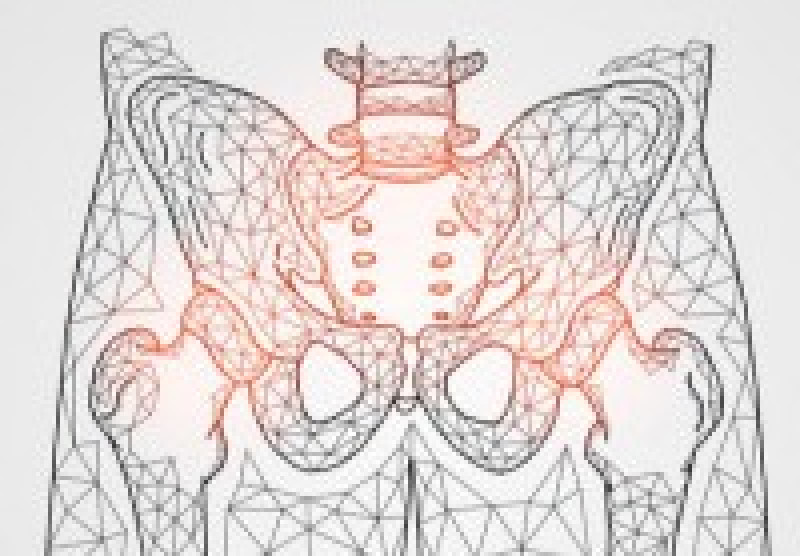
Anatomy of the Pelvis
The pelvis is made from two bones. The bones join in the front at the symphysis pubis and in the back with the sacrum at the sacroiliac joints. This forms a ring, and typically when a ring breaks, it will break in two places. The pelvis contains ligaments that help maintain the pelvic structure. These ligaments connect the sacrum to the iliac bones, the pubic bones to one another at the pubic symphysis, and the sacrum to the coccyx. Additionally, there is significant vasculature and nerves that run through the pelvis, which can cause severe hemorrhage, pain, and nerve damage if the patient experiences significant trauma.
Types of Pelvic Fractures
There are three categories of pelvic fractures, which range from most stable to least stable.
- Type A includes avulsion fractures, iliac wing fractures, and transverse fractures through the sacrum. These are stable and do not fracture through the pelvic ring.
- Type B includes open-book and lateral compression fractures. These are rotationally unstable but are vertically stable.
- Type C fractures are vertically and rotationally unstable.
Pelvic fractures can occur from several different types of injuries. They are broken into low and high-energy events.
- Low-energy events:
- Ground-level falls
- Avulsion fractures from sports
These types of fractures tend to be stable and occur typically in adolescent and elderly populations
During an assessment of the pelvis, the patient may feel stable, and we may not feel any crepitus, but it may be painful.
- High-energy events:
- Motor vehicle crashes
- Pedestrian vs auto crashes
- Falls from significant heights
These fractures tend to be less stable, and you may feel crepitus and instability when you are assessing the pelvis.
Management and Pelvic Fracture Concerns
Once we think our patient has a pelvic fracture, what should we do?
The first thing we want to do is try to stabilize the pelvis. Preventing movement reduces the risk that the vasculature and/or nerves running through the pelvis become damaged. Reducing movement may also minimize the amount of blood lost from bleeding bones (bones are highly vascular and can lose significant volumes of blood quickly). Patients can lose around 1-2 liters of blood with a pelvic fracture, so it is important to stabilize these injuries.
How do we stabilize the pelvis?
One simple solution is to tie a sheet around the patient's pelvis to hold it together. In the past, things like pneumatic anti-shock garments or MAST pants were used, but most places do not carry these anymore. Once you have stabilized the pelvis using a sheet, blanket, or pelvic splint, you should prepare to treat the patient for hypovolemic shock. As we cannot see the blood loss from pelvic fractures, it can be hard to estimate how much blood the patient is losing. Therefore careful monitoring of the patient's vital signs is critical. Hypovolemic shock is more common in unstable pelvic fractures than in stable fractures.
How do we minimize pain?
Pelvic fractures can be quite painful, and ambulances are not always the smoothest ride. Your patient will likely be quite uncomfortable during transport as you hit every tiny bump in the road. It is important to try to be smooth and gentle when loading and unloading your patient from the ambulance, as you do not want to jar the pelvis.
In summary, pelvic fractures can be dangerous and difficult to diagnose because they are internal. Thoroughly assess your patients on scene, especially elderly patients, and consider the mechanism of injury. Just because you cannot see it does not mean it is not there. Be sure to carefully assess the pelvis of an elderly fall patient, even if you are just called for a lift assist. If the patient has pain while standing and walking, which is unusual for them, bring them in to have imaging done. There can be significant or life-threatening damage even if the patient's pelvis feels stable.
In addition, just because a patient is young does not mean they cannot have a stable pelvic fracture. Adolescents are at risk of avulsion fractures to their pelvis from sports. If the pelvis is unstable, wrap it to increase stability and minimize bleeding. Lastly, frequently assess vitals to successfully identify early hypovolemic shock.
References
- Graf, K.W. (2016, July 19). Unstable Pelvic Fractures. Retrieved from https://emedicine.medscape.com/article/1247426-overview
- Russell, G.V. (2018, February 26). Pelvic Fractures. Retrieved from https://emedicine.medscape.com/article/1247913-overview
- Dozens of courses and topics
- State-specific requirements
- We report to CAPCE in real time


